Psilocybin Microdoses Show Promise in Easing Palliative Patient Distress
Researchers in Ottawa are expressing optimism about early findings from a groundbreaking study investigating whether microdoses of psilocybin can alleviate severe psychological distress in patients receiving palliative care. The novel research trial represents the first of its kind, aiming to determine if small, controlled doses of the psychedelic substance can effectively manage symptoms of depression, anxiety, and existential distress among individuals facing end-of-life challenges.
A Personal Journey Through Advanced Illness
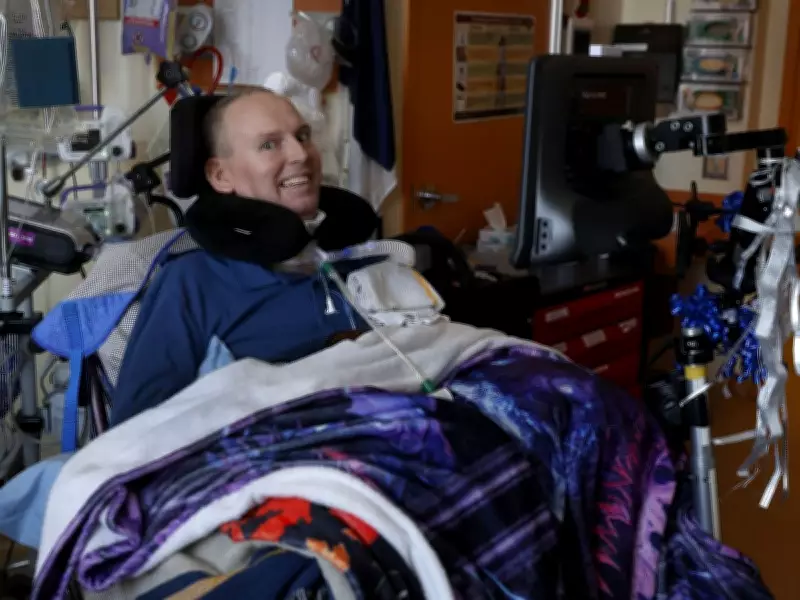
Andrew Chernysh, a 52-year-old military veteran and former cybersecurity specialist, has been living with advanced amyotrophic lateral sclerosis (ALS) for five years. Diagnosed with the neurodegenerative disease in 2021, Chernysh is now paralyzed from the neck down and relies entirely on a ventilator for breathing. He communicates using eye-gaze technology, which tracks his eye movements to spell out words and sentences on a computer.
After entering the palliative care program at Bruyère Health's Saint-Vincent Hospital in Ottawa during 2024, Chernysh initially expected to live only about one more year. Like many palliative patients, he experienced severe psychological distress—a condition affecting up to half of all individuals with advanced illnesses as they approach the end of life. At one point, he had signed a waiver of consent for medical assistance in dying and was seriously considering that option.
Today, however, Chernysh continues to look toward the future. When asked if he is happy, his eyes spell out "Y-E-A-H" on the computer. "I enjoy the simple things—the sun and visitors and activities," he adds through the computer-generated voice.
The Research Initiative and Its Objectives
Chernysh is participating in the pioneering research trial led by Dr. James Downar, a palliative physician at Bruyère Health and senior investigator at the Bruyère Health Research Institute. The study focuses on using microdoses of psilocybin to treat palliative patients who are experiencing severe psychological distress.
Dr. Downar explains that this type of distress is both common and notoriously difficult to treat in palliative settings. Standard medications for anxiety and depression often require weeks to take effect—time that many palliative patients simply do not have. "We really don't have particularly effective, scalable therapies for this," he notes.
The physician emphasizes that the distress experienced by these patients is not merely a result of inadequate support systems. "It is not caused by the fact that they can't get help. It is caused by the fact that they need it. They do not want people to help them. They want to be able to do it on their own," Downar states, highlighting the complex psychological dimensions of end-of-life care.
Broader Implications and Future Directions
The Ottawa-based research represents a significant step forward in exploring alternative treatments for psychological suffering in palliative contexts. While the study is still in its early stages, the initial results have generated cautious optimism among researchers and healthcare providers.
If proven effective through further research, psilocybin microdosing could offer a valuable new tool for palliative care teams struggling to address the profound psychological challenges faced by patients with terminal illnesses. The approach represents a departure from conventional pharmaceutical interventions, potentially offering more rapid relief without the side effects associated with traditional antidepressants and anxiolytics.
As the research continues to unfold, it may pave the way for more widespread acceptance and integration of psychedelic-assisted therapies within mainstream medical practice, particularly in settings where conventional treatments have proven inadequate for addressing the complex psychological needs of patients facing life-limiting conditions.









