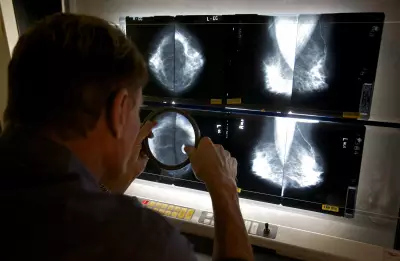
The Alarming Truth About Patient Dishonesty in Healthcare
If you resemble most individuals, you have likely stretched the truth during a doctor's appointment. This might involve underreporting your weekly alcohol consumption, exaggerating your exercise frequency, minimizing depression symptoms, or misrepresenting your willingness to take prescribed medication. According to a comprehensive study from the University of Utah, a staggering 60% to 80% of adults admit to lying to their physicians about their lifestyle habits and health behaviors.
Withholding the complete truth from your healthcare provider can significantly endanger your well-being, making such omissions particularly hazardous. Numerous factors drive this dishonesty: fear of judgment, anxiety about receiving a lecture, or apprehension regarding new prescriptions. Dr. Katie Freeman, an assistant professor at the University of Minnesota Medical School, notes, "People genuinely believe doctors will judge them and alter their treatment based on lifestyle information, whether good or bad. However, we truly do not have the time to judge. Our primary goal is to understand your situation to determine the appropriate next steps."
Concealing information from your doctor not only complicates their job but also jeopardizes your health. Below, medical professionals highlight the key topics patients frequently lie about and explain the serious consequences of such deception.
1. Medication Non-Adherence and Prescription Honesty
"One critical piece of information I always need to know is whether a patient is not taking their medication," emphasizes Dr. Raquel Zemtsov, an assistant professor at the University of Pittsburgh School of Medicine. This is a widespread issue; research indicates that up to 50% of individuals prescribed statins, a common cholesterol-lowering drug, discontinue use or fail to follow dosage instructions within the first year.
Dr. Zemtsov clarifies that learning about non-adherence does not disappoint her, but it fundamentally changes clinical decisions. "If you continue experiencing symptoms while I believe you are taking medication, I might devise a treatment plan that is unhelpful or unsafe," she explains. This could involve unnecessary additional prescriptions, extra diagnostic tests, or increased dosages. Patients should openly discuss any reasons for not taking medication—such as side effects, cost, or forgetfulness—so doctors can collaboratively find better solutions.
2. Transparency About Treatment Plan Concerns
Beyond medication, it is vital to communicate discomfort with any aspect of a treatment plan from the outset, according to Dr. Freeman. If you have experienced side effects, feel anxious about a recommended procedure, or intend to cancel it, informing your doctor allows them to address your concerns, provide reassurance, or suggest alternative options you are more likely to follow.
3. Accurate Reporting of Exercise and Dietary Habits
Humans often downplay behaviors they are not proud of, including inadequate exercise or poor dietary choices. Dr. Zemtsov warns, "If I am unaware that someone is not exercising or eating healthily, I may overlook related conditions like diabetes or high cholesterol." Similarly, if doctors assume you are meeting nutritional or fitness guidelines, they might not offer the necessary advice for improvement.
4. Full Disclosure of Substance Use
Many patients instinctively minimize their alcohol intake, smoking frequency, cannabis use, or illicit drug consumption when questioned by physicians. Both experts stress the importance of honesty, as substance use affects numerous health aspects, including sleep quality, cancer risk, respiratory function, and cognitive abilities. Dr. Freeman notes, "If you underreport drinking levels, I cannot provide accurate information about potential liver damage, blood count changes, or impacts on energy and mood."
Moreover, substance use often signals underlying physical or mental health issues. Dr. Zemtsov observes that it can be a coping mechanism for anxiety, depression, or pain. Understanding these motivations enables doctors to discuss substance risks and address root causes, potentially leading to effective interventions like therapy or medication.
5. Discussing 'Embarrassing' Bodily Functions
Patients frequently hesitate to mention bowel movements, urination problems, persistent diarrhea, or rashes in private areas. Dr. Freeman reassures, "People worry doctors will find these topics gross, but that is far from true." While discussing socially taboo subjects can be uncomfortable, physicians need this information to provide help. Online searches are no substitute for professional medical advice, which is safer and more private.
Ignoring such symptoms can be dangerous; for instance, bowel issues may indicate colorectal cancer, whose rates are currently increasing.
6. Openness About Sexual Health
Dr. Beth Oller, a family physician in Kansas, works to create an environment where patients feel comfortable discussing sexual health. "Often, when I ask about sexual health, it is the first time they have been asked, and they have assumed issues like painful intercourse or erectile dysfunction are inevitable," she says. Patients should feel empowered to raise these concerns, as sexual health problems can affect both physical and mental well-being and may signal other conditions, such as diabetes, heart disease, or autoimmune disorders.
If you cannot discuss sexual health openly with your current provider, it may be time to seek another physician.
Building Trust with a Primary Care Provider
Establishing a trusting relationship with a consistent primary care provider—whether a family doctor, internist, or pediatrician—fosters honesty and comfort. Dr. Freeman explains that repeated visits facilitate collaborative efforts to modify lifestyle habits. Dr. Zemtsov adds, "It is essential to find a primary care doctor who advocates for you and listens. Ultimately, we cannot help you unless we know everything about you."
For assistance with substance use disorders or mental health issues in the United States, contact the SAMHSA National Helpline at 800-662-HELP (4357).